IV Infiltration And Extravasation
Medical Malpractice Attorneys in Pennsylvania
Contact Frischman & Rizza Today
Frischman & Rizza, P.C.
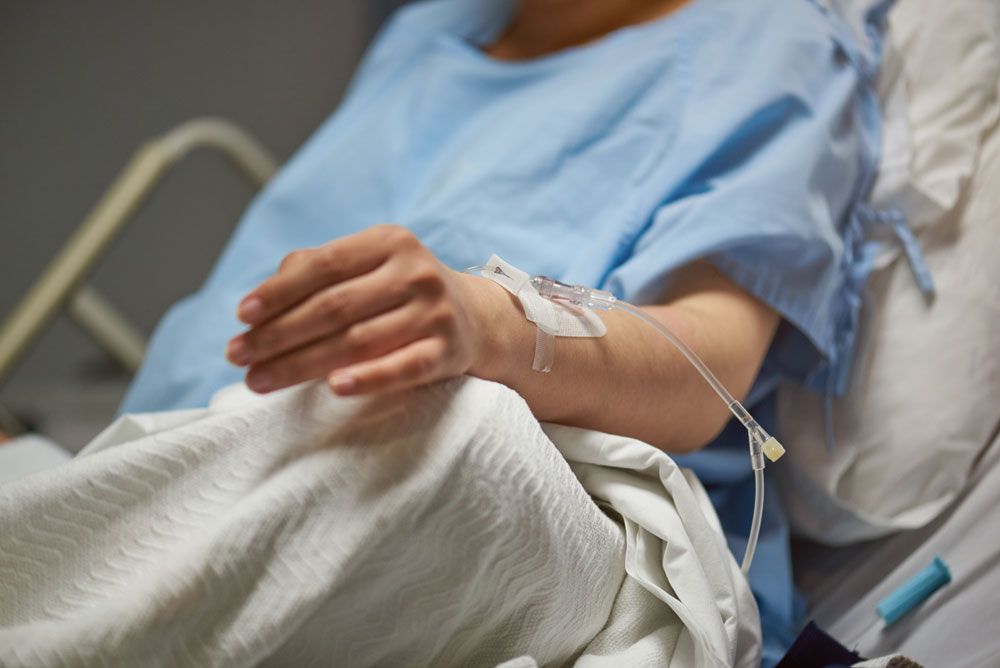
Quick Facts
An infiltrated IV (intravenous) catheter happens when the catheter goes through or comes out of your vein.
Some IV medicines can cause your skin and tissue to die (necrosis) if they leak into your tissues.
When this occurs it is referred to as an extravasation.
IV INFILTRATION AND EXTRAVASATION
The insertion of a peripheral venous IV catheter is a widely performed medical procedure in the United States. It has been estimated that over 200 million peripheral IV catheters are inserted into patients annually in the country, with approximately 70 percent of hospitalized patients receiving such lines during their admission.
Peripheral venous IV catheters serve as a secure method to deliver hydration fluids, blood products, and nutritional supplements to patients. Typically, veins in the arm are utilized as common insertion sites for peripheral IVs. The procedure itself is relatively straightforward and can be mastered through proper training and experience. It involves inserting a needle into the vein and sliding a plastic catheter (ranging from a larger 16 gauge to a smaller 24 gauge size) over the needle and into the vein. Once this is accomplished, the needle is usually removed, leaving the catheter in place as a conduit for delivering fluids. Compared to central venous IV catheters, peripheral IVs are generally used for shorter durations. Central venous IV catheters, on the other hand, are more complex to insert and are often employed for patients requiring long-term antibiotic or chemotherapy treatment. As a result, central venous IV catheters are typically inserted into larger central veins found in the chest and neck. While IV therapy offers convenience, speed, and safety in administering fluids, blood products, and medications, it is important to note that serious complications can occur, potentially leading to significant patient injuries.
Have you been injured?
Contact a Pittsburgh Personal Injury Attorney at Frischman & Rizza for a free case evaluation
Call Us On
Infiltration versus Extravasation
Although these terms are often used interchangeably, they represent very different complications from an IV catheter.
With both infiltration and extravasation, the fluid being administered to the patient leaks into the surrounding tissues as opposed to the vein in which the IV is inserted. This can occur for a variety of reasons, such as improper catheter insertion, catheter dislodgement and clot formation.
An extravasation occurs when a highly caustic solution known as a vesicant (one that can cause severe tissue damage or blistering), improperly infuses into the surrounding tissue as opposed to the intended vein. Many chemotherapy medications, antibiotics, nutritional supplements high in glucose concentration, blood pressure regulating medications, and electrolyte replacements are vesicants or have vesicant properties that can cause significant tissue damage if the solution improperly is infused into the soft tissues instead of the patient’s vein.
An infiltration occurs when a non-vesicant medication, such as hydration fluid, inadvertently infuses into the patient’s soft tissues instead as opposed to the intended vein. While clearly uncomfortable and can cause injury to the patient, an infiltration will not create blistering or burns.
To review, both an extravasation and an infiltration involves the accidental leakage of an IV solution into the surrounding tissue as opposed to the vein. It is simply the type of fluid that is being infused that distinguishes an extravasation from an infiltration.
Because of the potential for an extravasation or infiltration injury, the patient’s medical staff must be trained in proper IV line placement and regularly monitor the IV line to identify any signs or symptoms that the fluid is infusing into the surrounding soft tissues as opposed to the vein.
Prevention
Every medical institution where IV therapy is provided should have policies and procedures that address the manner by which a patient’s IV site needs to be assessed so as to prevent injury.
The Infusion Nurses Society publishes “Standards of Practice,” which many medical institutions adopt, require infusion nurses to be familiar with the fluid being infused into the patient. In particular, these Standards of Practice mandate that the infusion nurse be aware of the fluid’s potential adverse effects and those interventions that need to be implemented if an extravasation or infiltration occurs.
Before starting the infusion, the infusion nurse needs to assess the patency of the patient’s vein by checking for brisk blood return and lack of resistance when flushing the line. In addition to confirming vein patency, infusion nurses should avoid inserting IV lines into veins located in joint sites due to the increased risk of catheter dislodgement by movement. Also insertions into veins located in the hand and wrist should be avoided so as to minimize the risk to the patient of an inadvertent nerve injury.
After the IV has been placed and the fluid and/or medication begins to be infused, frequent site assessments must be performed. With non-vesicant fluids, site inspection for infiltration every several hours in an adult patient may suffice. However, pediatric patients should have their IV lines more frequently assessed for infiltration. When vesicant medications, such as many chemotherapy medications, certain antibiotics and nutritional supplemental high in glucose concentration are infused, the Oncology Nursing Society recommended site assessments be performed for signs of extravasation every 10-15 minutes because of their potential risk to the patient for significant injury.
Signs & Symptoms of IV Infiltration And Extravasation
Several of the most common signs and symptoms of an IV extravasation or infiltration include:
- Swelling, pain and/or redness at the infusion site.
- A sense of coolness often followed by a burning sensation in the surrounding tissue.
- Discoloration of the skin, such as blanching.
- Decreased flow of the fluid or medication being infused.
- Numbness, tingling or a pins and needle feeling in the area of the infusion.
Because of the potential serious injuries caused by extravasation and infiltration injuries, prevention and early detection is essential to patient wellbeing.
Injuries
Extravasation and infiltration can cause severe injuries that require extensive medical treatment and cause lifelong problems. If the extravasation of a vesicant solution occurs, the patient will likely suffer a significant burn type injury. This can cause tissue to be so severely injured (tissue necrosis) that the limb suffers severe functional issues and disfigurement. In rare situations, the limb where the extravasation occurred may require amputation. In virtually all cases of extravasation injuries, the patient will be left with tissue damage and scarring that requires extensive treatment.
If an infiltration occurs over a long period of time undiagnosed or if the patient experiences significant fluid leakage and swelling, Compartment Syndrome can occur. As discussed in the section of our website directed specifically to Compartment Syndrome, this is a very serious condition that can result in permanent nerve damage and tissue necrosis.
With both extravasation and infiltration injuries, nerve damage can occur. In cases of severe nerve injury, the patient can develop a devastating condition, called Complex Regional Pain Syndrome.
Because both extravasation and infiltration injuries can result in serious injury, the best treatment for extravasation and infiltration injuries is to prevent them from occurring.
Frischman & Rizza, P.C.
In Western PA Since 1992
Injured & Need an Attorney? Call Craig and Bernie!
- The Call Is Free
- The Consultation is Free
- We Don’t Charge A Penny Unless We Win Your Case!